
Geospatial Analysis of Tuberculosis Cases among Singapore Residents
Another piece of work that has taken much effort and a long time to get published (now out in Scientific Reports), but certainly one that expanded my own understanding of how diverse techniques can contribute to our knowledge of infectious diseases. This work – looking at the distribution of reported cases of resident (defined locally as “Singapore citizens” and Singapore permanent residents”) tuberculosis in Singapore via postal codes between 1995 and 2011 – was performed via collaboration with the Singapore Tuberculosis Elimination Programme (STEP) Registry and statistical modellers from the Saw Swee Hock School of Public Health. In particular, the lion’s share of work was performed by Dr Sourav Das, a former postdoctoral fellow at SSHSPH and who is now based at the University of Bristol, and A/Prof Alex Cook (who appears ubiquitous in Singapore in infectious diseases modelling work).
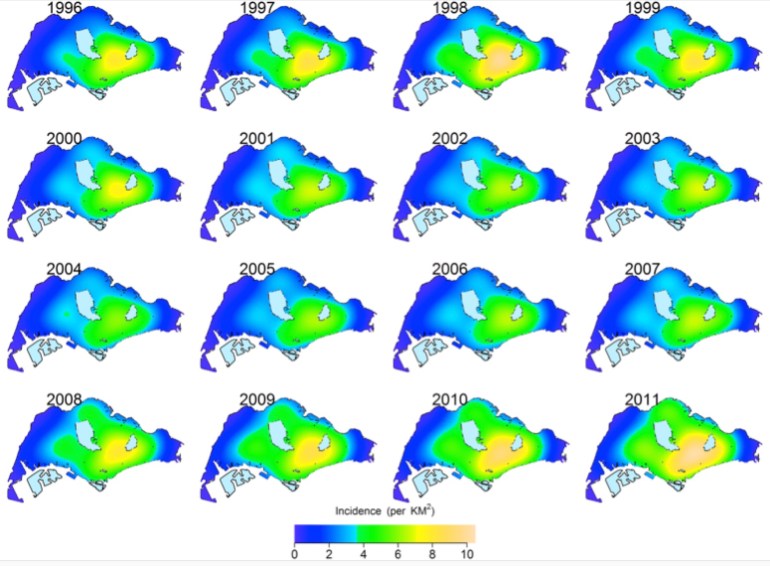
Annual spatial intensity maps of “risk of tuberculosis” in Singapore. Dark yellow signifies high intensity areas, fading to blue as the risk falls.
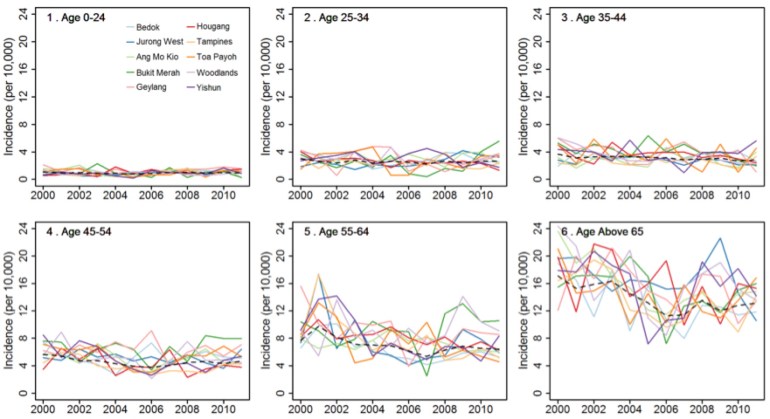
Resident annual time series incidence of tuberculosis across different age groups in Singapore, with incidence adjusted for underlying susceptible population.
Using geospatial analysis to look at tuberculosis is a different way to look at clustering of cases, and ideally should be combined with other techniques such as classical “shoe leather” epidemiology and molecular fingerprinting in order to provide granular understanding of the spread of the disease. Nonetheless there were still several interesting observations, taking into account the underlying population geospatial distribution:
- The southeastern planning areas of Singapore saw consistently high concentrations of tuberculosis cases between 1995-2002, but there was rising spatial intensity in all areas between 2008-2011.
- As residential development occured in the western planning areas of Singapore, there was a rise of spatial intensity of tuberculosis in these areas.
- We did not find any significant residential clustering of non-resident cases in neighbourhoods with a high number of resident cases.
- Stratifying by age groups (figure above) showed that the incidence of tuberculosis generally fell or remained the same across all age groups, suggesting that the recent rise in incidence of tuberculosis in Singapore is – at this point in time up until 2011 – largely driven by an ageing population.
The problem with the study is that we were not able to perform similar analysis for the non-resident population of Singapore. Statistics for the non-resident population, such as breakdown by ethnicity or age, or where they are distributed among Singapore’s planning zones, are not available publicly. Not being able to apply more refined analysis because of the lack of molecular fingerprinting information for the majority of cases was another limitation.