Clinical Vignette 25
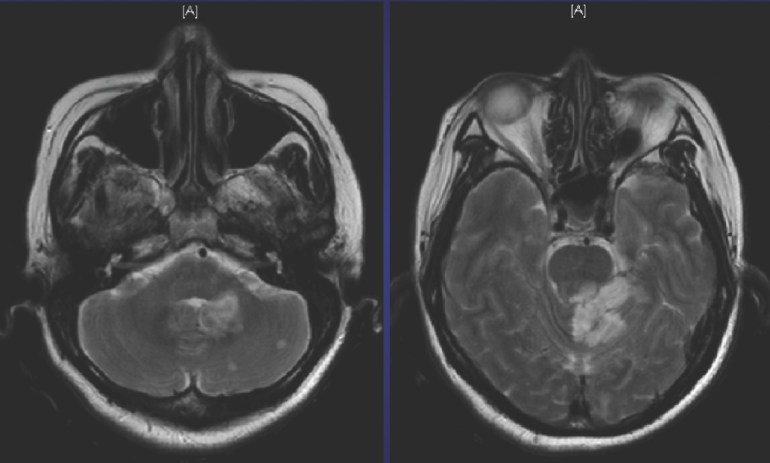
A middle-aged housewife with a history of chronic eczema and penicillin allergy (“rash and eye swelling”) presented with 2 days of fever, chills and lethargy. The initial clinical examination was unremarkable except for ongoing eczema and fever. The initial laboratory tests were remarkable only for mild thrombocytopaenia (114) and neutrophilia. However, she had chest pain 3 hours into hospitalisation, with mildly elevated cardiac enzymes (Troponin T = 0.55 ng/ml; normal CKMB), followed the next day by increased drowsiness with right gaze preference and mild neck stiffness. Repeat clinical examination in the intensive care unit (ICU) revealed a systolic cardiac murmur at the left sternal edge and a septic spot in her conjunctiva. An urgent MRI brain was arranged, showing multiple acute brainstem and cerebellar infarcts.
Within 24 hours, the blood cultures were positive for methicillin-susceptible Staphylococcus aureus.
Question: What is the diagnosis and what would be the plan of management (note that this case took place in the pre-daptomycin era)?
[Updated 28th March 2015]
Given the blood culture of MSSA, cardiac murmur and the multiple embolic phenomena (conjunctival septic spot, brainstem and cerebellar infarcts), the diagnosis of MSSA infective endocarditis is highly likely. An echocardiogram (trans-oesophageal echocardiograms or TEEs have greater sensitivity and are generally recommended for MSSA bacteraemia) should be performed urgently, and surgical management (i.e. valve replacement) entertained if a large vegetation or valvular abscesses are found.
Antibiotic treatment is rather complicated here because of the history of penicillin allergy (and possibly anaphylactic reaction given the eye swelling described). Unfortunately, the beta-lactam antibiotics are far superior to vancomycin for the treatment of severe MSSA infections. Currently, we have daptomycin, which would be the drug of choice here. In the pre-daptomycin era, or if the drug was for some reason not available, the best option would be to start the patient on vancomycin, but then to perform a rapid penicillin de-sensitisation under close monitoring. In the past, an aminoglycoside such as gentamicin would also have been added for “synergistic activity”. However, we now understand that combination therapy in this scenario leads only to increased risk of renal toxicity, but does not improve mortality nor other clinical outcome measures.