Clinical Vignette 57
A young local woman who was previously well went on a 9-day missionary trip to Pakistan, traveling between Karachi and Lahore as well as several villages in between. She had an episode of fever with chills midway through the trip, associated with diarrhoea two days later. Although the diarrhoea improved over the next two days, it never stopped, not even upon her return to Singapore. The diarrhoea was non-bloody and watery, occurring at least 4-5 times each day. She had no further fever and her appetite remained good. A short course of oral ciprofloxacin provided by the polyclinic doctor had not helped. Stool cultures done at the polyclinic were also negative. Her polyclinic doctor had apparently told her to “wait it out” but her symptoms persisted for close to 4 weeks without any improvement. A special stool test was ordered.
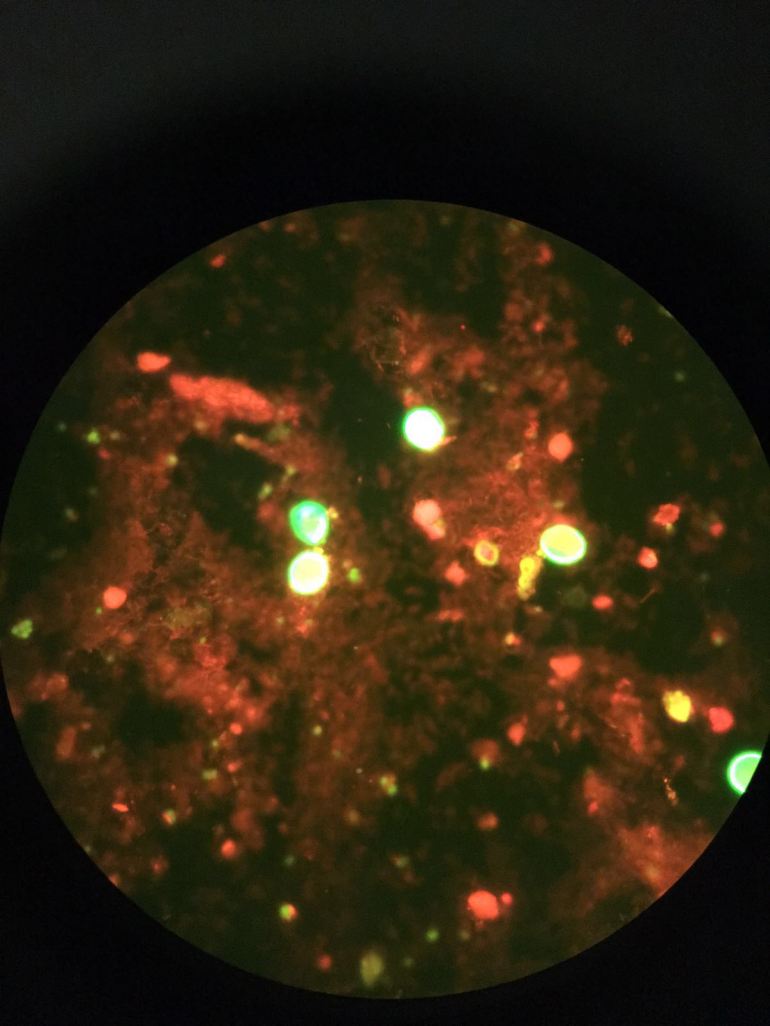
Immunofluorescence microscopy of stool. Larger “particles” here are approximately 8-10 micrometers in diameter (image courtesy of Diagnostic Microbiology, SGH).
Question: What are the diagnoses and what treatment should be offered?
[Updated 28 March 2016]
It is not a straightforward diagnosis by microscopy (unless one is a microbiologist), but the clinical presentation and treatment history provide reliable clues. This lady had chronic diarrhoea after traveling through rural parts of a developing country, and the illness did not respond to the usual oral ciprofloxacin. It is quite likely that she had chronic diarrhoea from parasitic infection, and – as with STD’s – such infections can be caused by multiple parasites at the same time. In this case, the larger particles are Giardia lamblia cysts, while the much smaller particles are Cryptosporidium spp. The former can be treated with a short course of oral metronidazole with good outcomes. The latter is far harder to treat, partly because medical treatment does not work as well, and partly because the drug that is used – nitazoxanide – is not easy to acquire in Singapore. Paramomycin has also been tried for “crypto” diarrhoea, but does not work as well.