Clinical Vignette 60
A middle-aged man was recently diagnosed with poor prognosis myelodysplastic syndrome (MDS). He was prescribed a course of subcutaneous azacitidine. One week after the first cycle (7 days) of the drug, he presented with pain over the injection sites (over his anterior abdominal wall), associated with high fever and weight loss. He was admitted to hospital 2 days later when his symptoms failed to abate with oral augmentin.
On clinical examination, he appeared ill, having rigors, and a temperature of 39 degrees Celsius. His abdominal wall was inflamed and tender, with no underlying fluctuance. He was started on broad-spectrum antibiotics and an IV drip. CRP was 287 mg/dL and procalcitonin was elevated at 1.3 mcg/L. Two days later, blood cultures remained negative and his fever continued unabated. The abdominal wall inflammation had extended, with a central area of necrosis in one lesion.
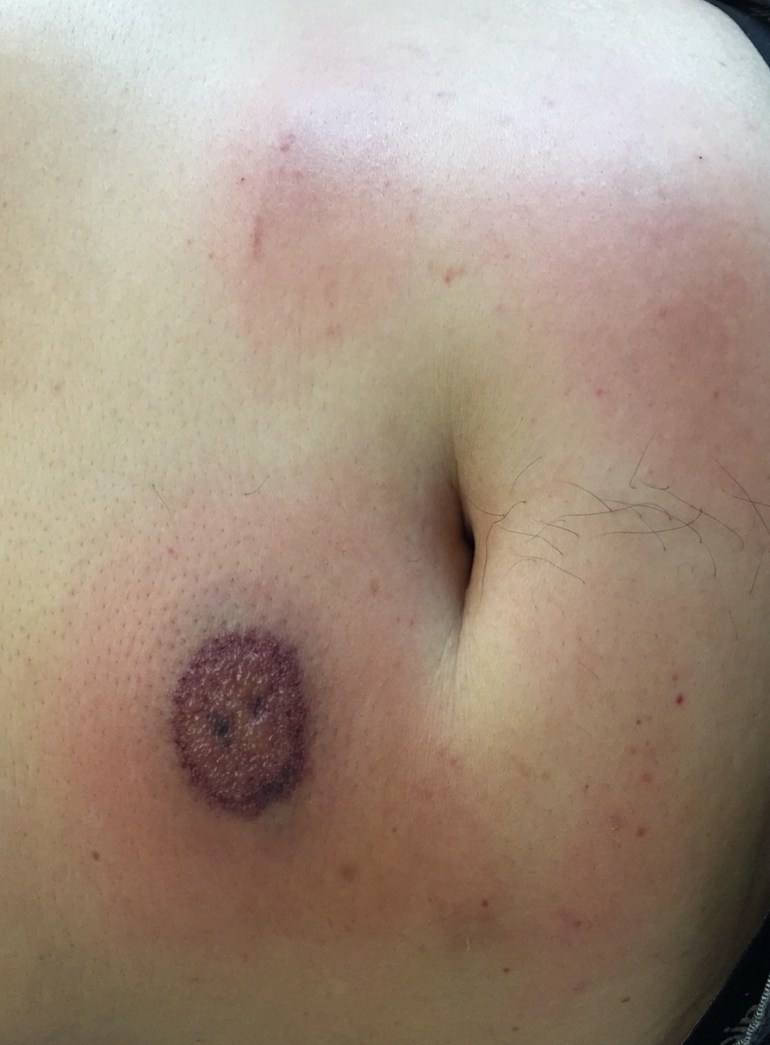
Question: What is the likely diagnosis and how should this be managed?
[Updated 26 June 2016]
This is actually a local and systemic reaction to azacitidine – azacitidine-associated neutrophilic dermatosis. It presents almost exactly like severe cellulitis (and even necrotising fasciitis), but cultures are invariably negative and antibiotic therapy does not help. Histology (of affected skin) is sometimes unhelpful as well. Inflammatory markers (i.e. Procalcitonin, C-reactive protein and ESR) are almost always raised.
The key is not to persist with ever-escalating types of antimicrobial agents, because a delay in appropriate treatment can be life-threatening. This condition will respond to systemic steroids.