
Clinical Vignette 78
A late middle-aged gentleman presented with painful left knee swelling for 2 weeks. He had recently been diagnosed with primary autoimmune hemolytic anaemia, for which he was on the final week of a 12-week tapering course of high-dose prednisolone.
There was no associated fever or other systemic symptoms. He had not traveled in the preceding 6 months, and did not keep any pets. A fall off a bike 3 months prior to the knee swelling had resulted in superficial scratches on both knees that healed without incident.
On examination, the left knee was swollen and warm, particularly over the medial aspect, where a little pustule was apparent. Range of movement was limited by pain.
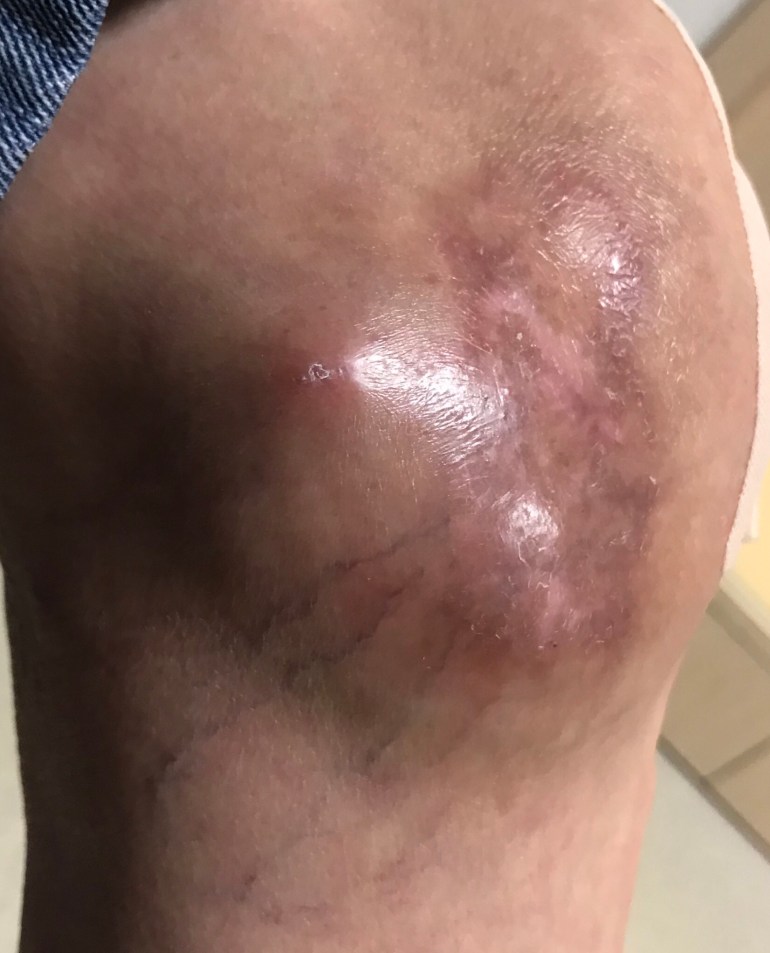
An arthroscopic washout was performed, revealing inflamed synovium and pus in the knee joint. Microscopy of the pus showed predominantly lymphocytes, with scanty acid-fast bacilli seen. TB PCR was negative, however. Mycobacterial cultures – 3 days after the procedure – were still pending. Chest X-ray was clear.
Question:
- How should this patient be treated?
[Updated 5th November 2017]
Difficult as it is, because the infection is localised, it is probably best to wait for the culture result. A negative TB PCR in the presence of positive AFB smears effectively rules out TB, but there are many different non-tuberculous mycobacteria (NTM) that can cause such an infection, especially in an immunocompromised patient who had received a long course of corticosteroids. The treatment for each NTM can be different, and prescribing a cocktail of drugs to cover the more common NTM often results in drug adverse effects. It is not easy to explain such “inactivity” to the patients however.
In this particular case, synovium cultures eventually grew Mycobacterium haemophilum, for which he received rifampicin, clarithromycin and ciprofloxacin for a prolonged duration.