Dengue Infections, Singapore
For the past several weeks, dengue has been in the news because of the surge in cases – the highest for the past several years.

The National Environment Agency (NEA) has attributed this to three main factors:
- An increase in the Aedes aegypti (the primary vector for the dengue virus in Singapore) population in Singapore.
- Warmer weather (June to October being the usual months where dengue cases rise each year).
- Low herd immunity in Singapore.
A recent Channelnewsasia article highlighted different opinions among other experts, however, ranging from “dengue phases of 3 to 4 years”, increase in construction sites locally, changes in “sub-serotypes” of dengue, and viral evolution.
A look at past reported cases also seems to suggest that the incidence of dengue had increased dramatically in the 2000s. For example, in this Infopedia article, the first outbreak of dengue reportedly occurred in 1960 (88 cases), whereas 1973 “saw one of the largest outbreaks in history” with 1,324 cases and 27 deaths.
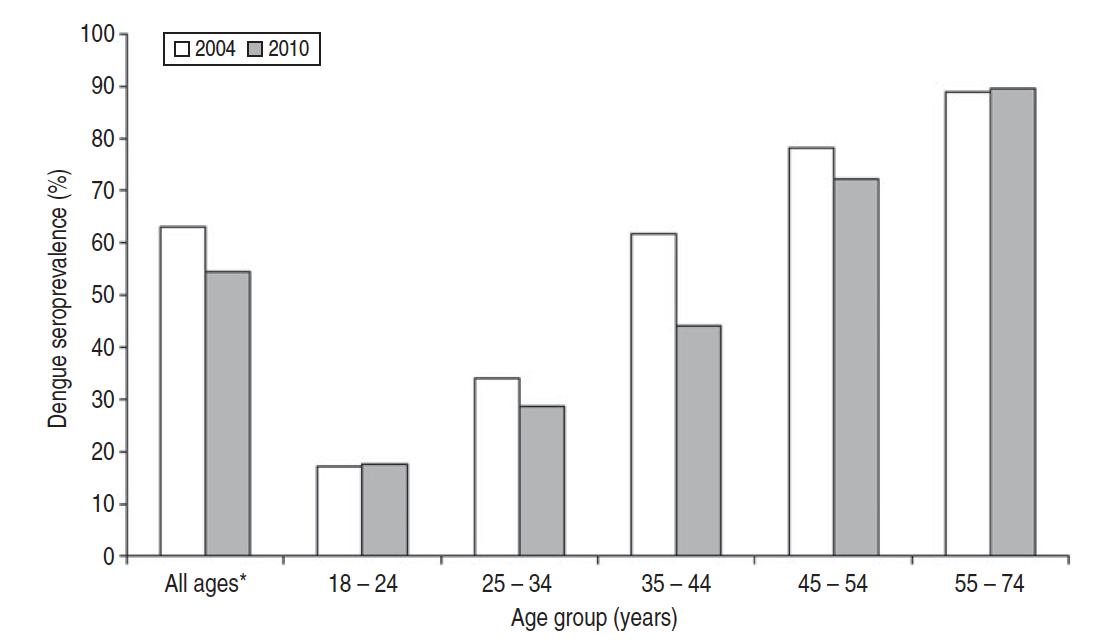
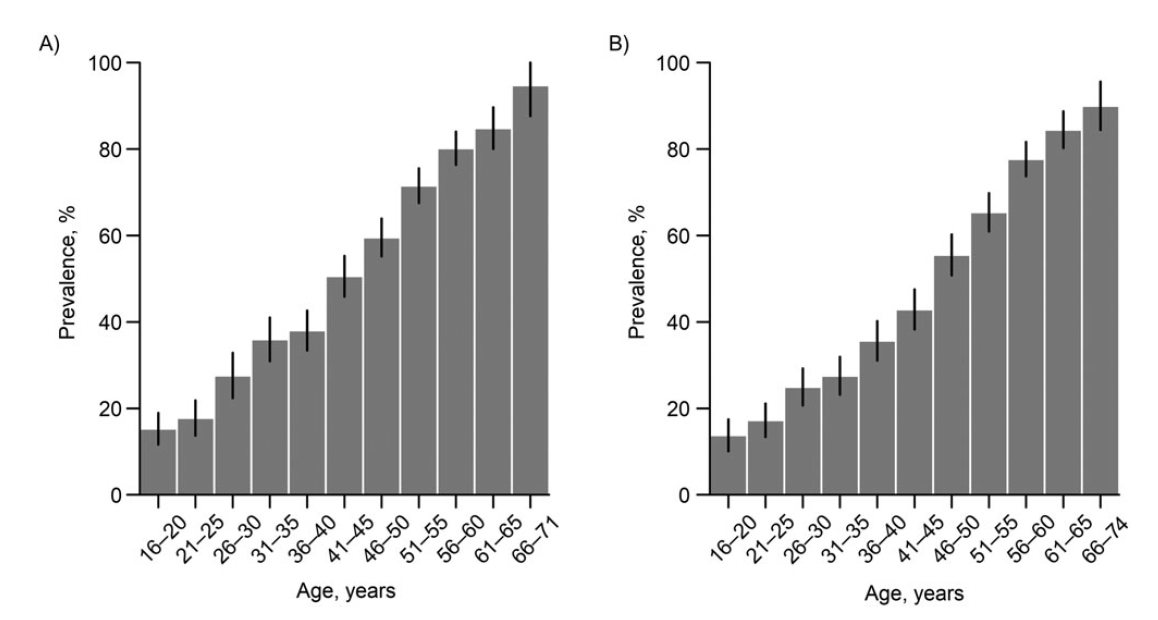
Since 2008, however, there have been a number of dengue seroprevalence studies published as well as estimates of “force of infection” of dengue over the years. The epidemiological term denotes the rate at which susceptible individuals acquire infection, and is used comparatively across time or between diseases. These consistently highlight a startling result: dengue infections were far more prevalent in the distant past, and the dengue “force of infection” had decreased significantly since the 1960s, with a slight blip in the 2000s. The results from the several serosurveys (1982, 1998, 2004, , 2009, 2010, 2013 and 2017) are shown below as screenshots from the respective articles: Low SL et al (2015); Ang LW et al (2015); Tan LK et al (2019).

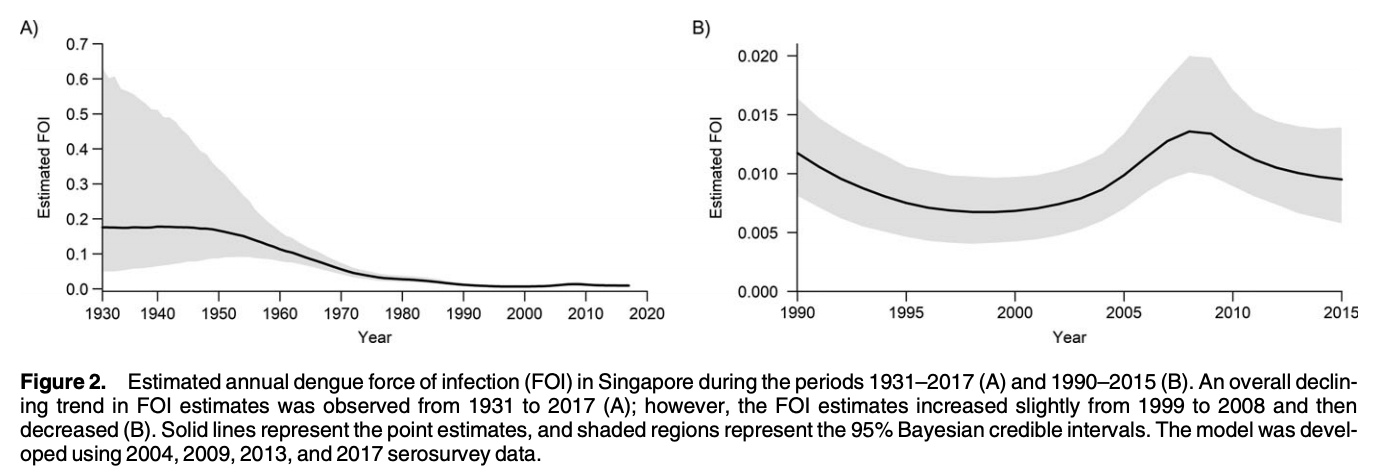
The dengue “force of infection” in Singapore over time was last estimated recently, including data up to 2017, and I have included the screenshot of the chart below. Note that prior to the 1960s, there are no real data and the confidence intervals for the mathematical model is very wide. It is generally similar to the earlier estimation in 2008, with virtually a tenfold fall between the 1960s/1970s and the past two decades.
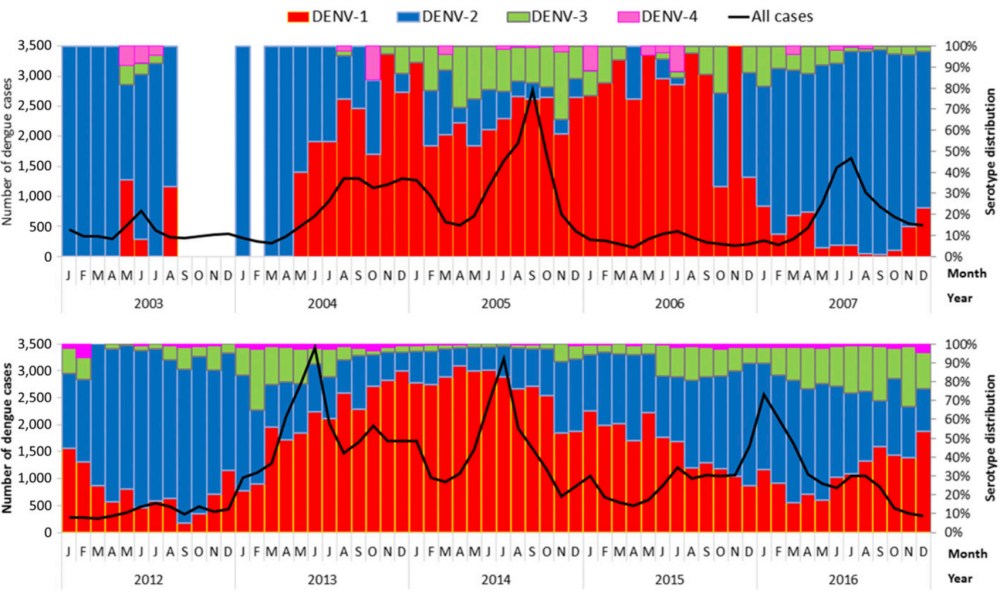
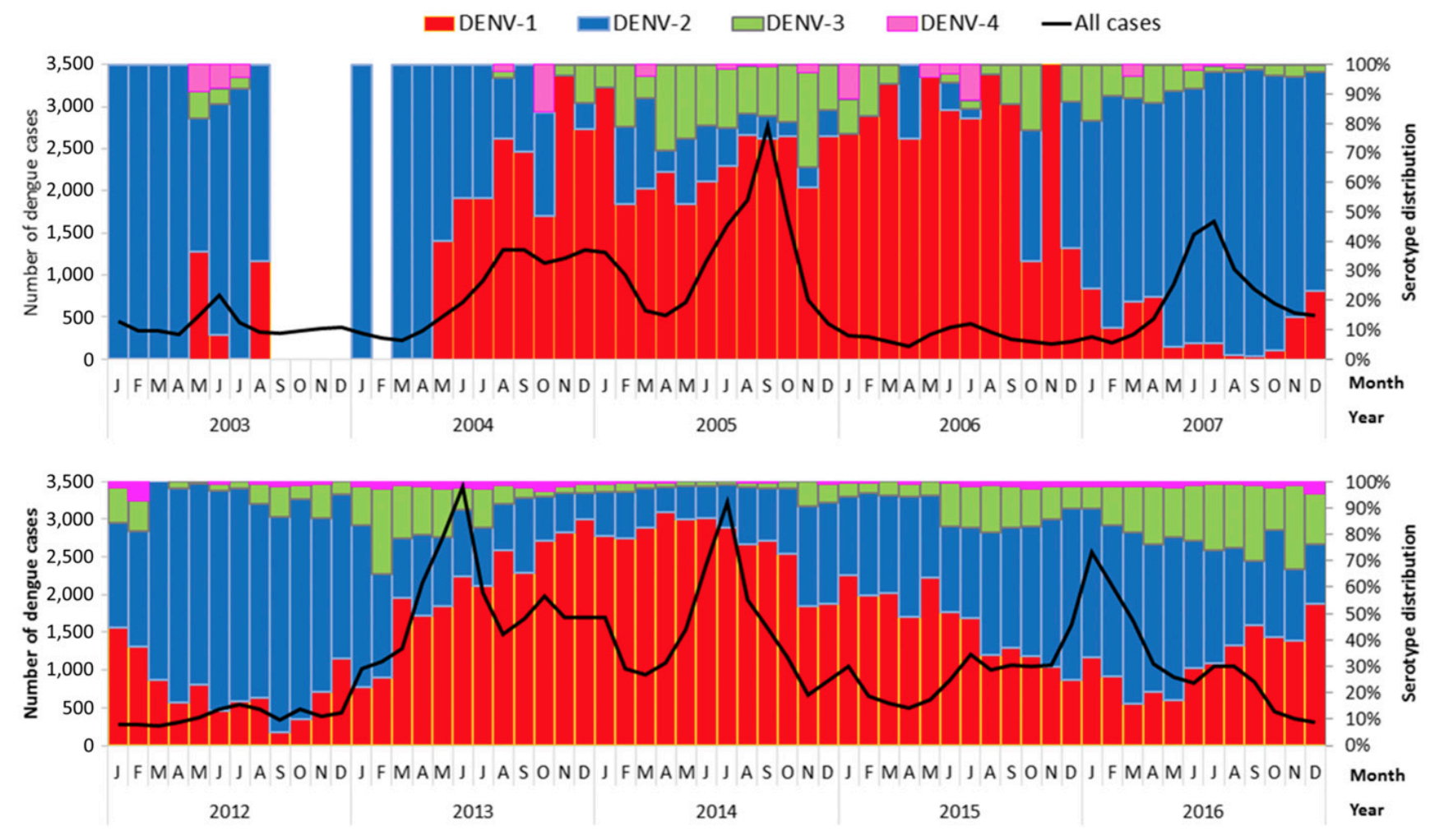
How about the theory of serotype switches resulting in cyclical outbreaks? In Singapore, the primary dengue serotypes have been Den-1 and Den-2 since serotyping have been performed, with a smattering with Den-3 and Den-4. Certainly this would not seem to be a sufficient cause for any significant surge in cases, given the large proportion of susceptible individuals in the population.
One final interesting but controversial point: for decades (and I was certainly taught this in medical school and during ward rounds), it was believed that dengue infection resulted in lifelong immunity to that specific serotype of dengue, so in theory each individual could be infected four times in his or her lifetime. In 2016, however, a pair of papers published from studies in Nicaragua and Peru showed that homotypic (i.e. repeat infection with the same serotype) dengue infections could and did occur. So it is plausible that a small but significant proportion of infections locally have occurred as a consequence of re-infection by the same serotypes (DEN-1 and DEN-2).
I’ve always thought of a serotype switch as being the *result* of an outbreak rather than the *cause* of an outbreak: as you note, the serotypes are always present even if at low levels, and immunity levels in the population don’t change much from year to year, so the ingredients are always there for any serotype to take off. When it does, then we look back and see that it was mostly of one serotype, which we posthoc label as a ‘serotype switch’.
The paper by Tan et al (2019) also points out that the seroprevalence and incidence of reported cases can only be reconciled by greater reporting of cases. They report that the notification rate has risen from about 1 in 14 to 1 in 6 infections over the last decade. It’s ironic that better work by doctors makes it look like public health is doing worse.
Another reason not mentioned in your blog but which is sufficient to explain outbreaks like the present one is pure chance: I’m sure we can all accept that the number of cases goes up and down in a semi random fashion, but if we formalise this within a simple model, the patterns we observe in Singapore are similar to those we observe in simulations from a purely random process in terms of frequency and magnitude of outbreaks (Chen Yirong’s paper from EID from a few years ago). So perhaps we don’t need to expend too much effort in seeking explanations of why there’s an outbreak unless it is substantially bigger than the current one.
LikeLiked by 1 person