Clinical Vignette 45
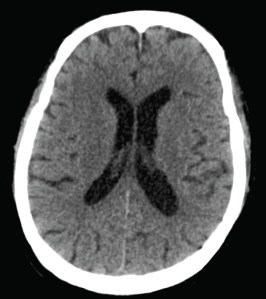
A middle-aged (late 50’s) housewife presented with fever for 4 days, associated with headache and photophobia. There was no significant contact or travel history, and her only chronic medical condition was hypertension for which she was on atenolol (a beta-blocker). Brought in to the emergency department by her husband and son, she was found to have a fever of 38.9 degrees Celsius, neck stiffness, and appeared mildly disoriented, answering questions appropriately but rather slowly. Her blood pressure was “normal” at 150/84 mmHg, and no neurological deficits were found on clinical examination. A CT head was done, which was normal (sample cut below).
Question: What is considered optimal management for this woman? And why is it not usually implemented?
[Updated 17th September 2015]
Recent events (i.e. the Singapore elections among others) have resulted in this tardy update, for which I apologise.
This is a straightforward case of suspected meningitis, and the key principles are:
- Early lumbar puncture in order to obtain CSF for diagnostic tests (including cell count, CSF biochemistry, and the relevant cultures/molecular tests).
- Early institution of empirical antibiotics.
- Concurrent administration (15 minutes before and up to the timing of the first of dose intravenous antibiotics) of steroids.
Unfortunately, this is not regularly done in many parts of the world, including Singapore. Locally, the barrier(s) seem to be at the level of the Emergency Departments (ED’s). Whereas CT scanners are now located within most of the ED’s in Singaporean hospitals, and CT heads can be done very quickly, lumbar punctures are virtually never done in the ED setting for a variety of reasons. I suspect it is largely to do with time (ED’s are perpetually busy with long queues of patients – and a lumbar puncture takes time to organise and perform), the rarity of bacterial meningitis in Singapore, and perhaps the remuneration system. That flat SGD115 or so for an ED consult – while it seems like quite a bit of money – hardly pays for the CT and the lumbar puncture, not withstanding the actual diagnostic tests that need to be done, although there are workarounds.
Most of the patients do get their antibiotics (without the lumbar puncture) at the ED’s, but not the concurrent steroids – a Catch-22 situation: the lumbar puncture has not been done, so a diagnosis of meningitis cannot be confirmed, and hence steroids cannot be given. I am not sure if there is actually a way to move forward with this in order to deliver optimal care for patients with meningitis that present at local emergency departments.
Probably lumbar puncture, empirical Antibiotic therapy, even to include coverage for herpes virus. Adjust after results of the lumbar puncture.
It’s usually not done because lumbar puncture is thought to be too invasive and there are cultural concerns about it.
LikeLike