
Separation of Drug Dispensing and Prescribing
This issue came up as part of a discussion on improving antibiotic prescription – the discussion triggered (strangely enough) by the lack of mention in this week’s Straits Times article on inappropriate antibiotic prescription.

It is an interesting topic for discussion and understanding, but I would like to stress that the issues go far beyond “mere antibiotics”, and the desire to curb the rise of antibiotic resistance should not be used as a key reason to consider such a policy. The political costs are too high. Dispensing and prescribing are not just healthcare matters, but in many ways cultural and social issues as well.
Currently, there is no policy for the separation of drug prescription and dispensation rights in Singapore. The issue of separating drug prescribing from dispensing came into public attention in January 2005 in a series of Straits Times articles (it is hard to find them now, but Dr Gerald Tan has kept a detailed account on his website here), with the Ministry of Health and therefore mainstream media occasionally re-surfacing the issue (the aforementioned account by Dr Tan extends to news articles in 2007). But an article on the Pharmaceutical Society of Singapore’s website suggests that the issue had been rumbling on since at least the late 1980s.
It is important to note the global context: the majority of developed countries/regions have implemented policies that separate drug dispensing from prescribing, including neighboring countries/regions such as Japan, South Korea and Taiwan. There are caveats and exceptions to these policies – in rural parts of countries, exemption from separation of these “powers” are granted. The journey to enact such policies in Malaysia began in 1973 and appears to be unsuccessful at this current time (article behind a paywall), with several acrimonious letters published in the mainstream Malaysian media.
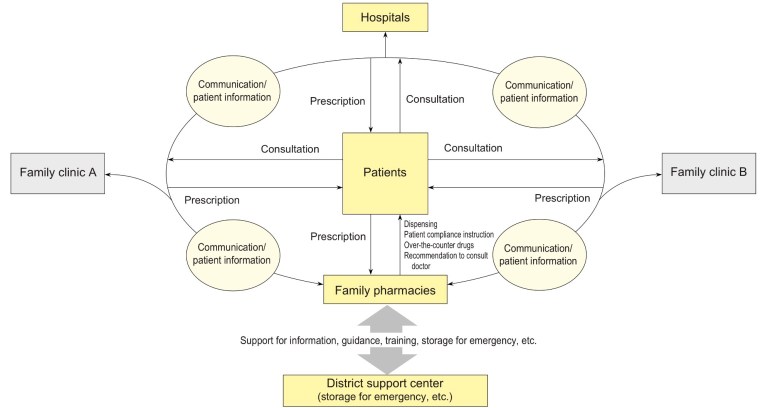
Screen capture: Japan’s system – from http://www.mhlw.go.jp/english/wp/wp-hw4/dl/health_and_medical_services/P99.pdf
There are clear advantages and downsides to either position, and these have been articulated in several reputable articles (a very lengthy one here) without the accompanying rhetoric and posturing one often finds in physician and pharmacist writings (both groups have powerful lobbies and significant interests at stake). It is incredibly convenient to be able to get a physician consultation and collect medicines at the same location. If GP and specialist clinics are not allowed to dispense medications, consultation fees will inevitably rise sharply, and tremendous public sector investment is required in order that the total cost for seeing a doctor and getting medicines should remain cost-neutral for individual patients. However, physicians having their own “pharmacies” and profiting from dispensing creates a situation where there are significant perverse incentives, something which multiple organizations including WHO warns against.
A personal anecdote: when I was running my own “mom and pop store-style” specialist clinic, I also kept a small cabinet of drugs (mostly antibiotics) and vaccines to dispense. It was impossible to be completely free of awareness as to when the drugs were expiring, or thoughts of whether “in-house” drugs could be effective substitutes for those that were available only elsewhere.
One final point from all the reading. Reforms that led to the separation of prescribing and dispensing in most countries – especially those from our part of the world – took decades to become law and to be implemented. The outcomes were (of course) never as rosy as painted by supporters of separation, but not as apocalyptic as suggested by their opponents either. And sometimes social practices developed that were unanticipated and outside of policy intentions. In the case of Taiwan for example, health expenditure did not decrease, and the elderly appeared more inclined to visit physicians who had hired on-site pharmacists.