
Clinical Vignette 81
An elderly man presented with fever and malaise for a week followed by right buttock pain which was worse on sitting for 2 days. He has well-controlled hypertension and ischemic heart disease.
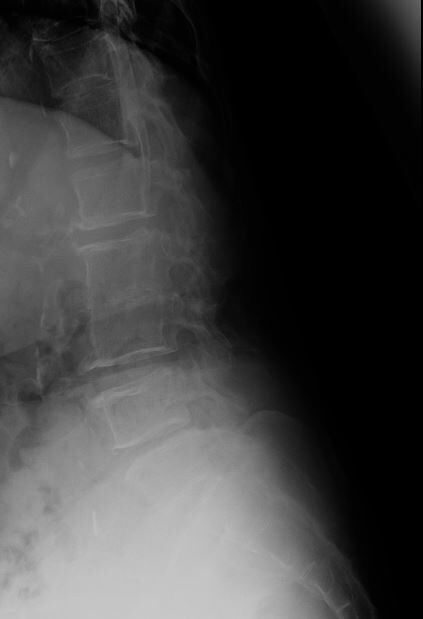
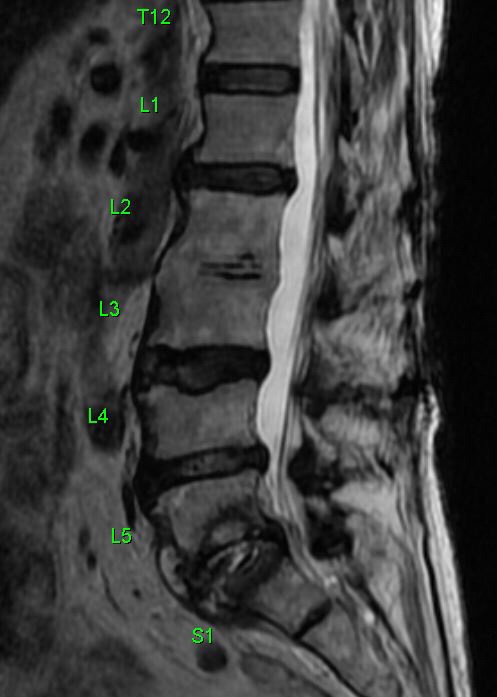
An X-ray of the lumbosacral spine showed narrowing of the L2-L3 disc space following which an MRI of the spine was arranged. Blood cultures were positive for Streptococcus bovis.
Questions:
- What is the diagnosis?
- How should this man be managed?
[Updated 24 February 2018]
The MRI showed degenerative changes at L2-L3, but more importantly, spondylodiscitis at S1-S2, with impingement of nerve roots (which would explain the symptom of buttock pain. This is most plausibly attributed to the Streptococcus bovis bacteremia.
The organism (which is now classified as S. gallolyticus biotype bovis) is associated with two conditions – infective endocarditis and colorectal cancer. Therefore this patient should be strongly recommended colonoscopy to determine if there are colonic lesions, and echocardiography. Management of the infection is with high-dose intravenous penicillin, with a prolonged antibiotic duration of at least 4 weeks.
Many would recommend an echocardiogram reflexively even if there were no cardiac murmurs or other signs/symptoms of endocarditis. Given the cost of the investigation (transthoracic echocardiography is relatively risk-free but costs several hundred Singapore dollars), and the fact that the patient will in any case require prolonged antibiotics, the need for this investigation is indeed worth discussion. An echocardiogram can however impact treatment decision – the treatment of endocarditis would require weeks of high-dose IV penicillin (other antibiotics like ceftriaxone are equivalent alternatives, but nonetheless still IV), whereas oral antibiotics with good bone/joint penetration can be used to treat the spondylodiscitis.
infective endocarditis complicated by vertebral osteomyelitis via haematogenous spread?
he needs an echocardiogram to assess the severity of the valvular involvement, and IV penicillin + gentamicin (if the MIC of the streptococcus is susceptible). should also consider the need for colonoscopy as it is associated with colon cancer.
LikeLike
Great!
LikeLike